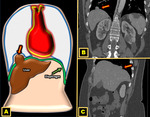
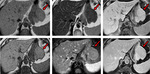
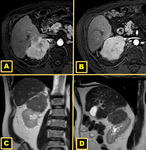
Classification of ALL
The accessory lobes of the liver vary in size and topography,
and the liver tissue is often connected to the main organ,
although cases of ALL completely separate of the normal liver have also been reported.
Another entity to be considered is ectopic hepatic tissue,
which is situated outside the liver without any relation to it,
usually attached to the gallbladder or intra-abdominal ligaments.
These ectopic tissues can also be found anywhere in the thoracic,
abdominal,
or pelvic cavities 1,7 Fig. 2.
There is a classification of ALL,
according to Stattaus et al.,
which divides the entity into two types: a) an accessory lobe attached to the normal liver or b) a completely separate accessory lobe 8.
ALL can also be classified as pedunculated,
sessile or ectopic.
There are several types of ALL that are classified by volume and weight 9:
- A bulky ALL (> 31 g) connected to the liver via a stalk of tissue or a wide base in the subphrenic or perihepatic zone;
- A small ALL (11-30 g) connected to the liver via a wide base on the hepatic surface or around the right posterior lobe;
- A completely separate ALL with no connection to the liver that is most often seen in the thorax or pelvic cavity;
- A pinpoint ectopic ALL (< 10 g) that is most often located at the margins of the liver or even of the gallbladder wall.
There is another method of classification of ALL in three types based on its biliary drainage and the presence or absence of a common capsule,
as proposed by some authors 9:
- Type I - The separate accessory lobe duct drains into an intrahepatic bile duct of the normal liver.
- Type II - The separate accessory lobe duct drains into an extrahepatic bile duct of the normal liver.
- Type III - The accessory lobe and the normal liver have a common capsule; the bile duct of the accessory lobe drains into an extrahepatic duct.
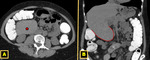
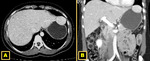
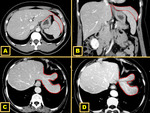
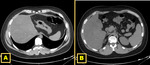
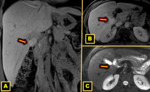
Abdominal ALLs,
and especially right abdominal ALLs,
are more commonly reported than those ALLs located in the thorax or pelvic cavity,
which are rare 10 Fig. 3.
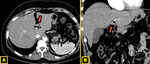
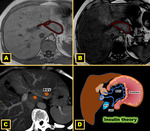
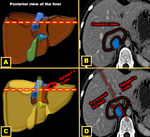
Riedel’s lobe
Riedel's lobe (RL) is the most well-known type of ALL and was described in 1888 for Riedel as a tongue-like elongation of hepatic segments V and VI,
located in the right upper quadrant and that may extend into the right flank and iliac fossa.
However,
there are cases in literature reporting RL in the left lobe,
although this is not the rule.
They can be sessile or pedunculated according to their type of attachment to the liver,
and even ectopic 6 Fig. 4.
RL must be distinguished from the ‘‘Corset Liver’’,
characterized by a deep fibrous groove on the anterior aspect of the convexity of one of the two lobes,
resulting from chronic compression of the liver by a corset,
a belt or a skeletal deformity 6.
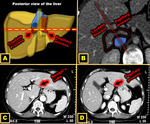
The prevalence of RL,
as determined mainly from radiological series,
ranges from 3.3% to 14.5% in the literature,
and the prevalence is higher in women than in men.
The wide range of prevalence possibly underscores the existence of several definitions in the literature and the absence of standardization of diagnostic criteria on imaging 6 Fig. 5.
The diagnosis of accessory liver lobes
ALL is rarely seen clinically and is difficult to diagnose before surgery.
It is often misdiagnosed because most patients with an ALL have no symptoms.
Many cases of ALL were misdiagnosed as an intraperitoneal tumor,
pulmonary tumor,
or diaphragm tumor 10,11 Fig. 3 Fig. 6.
With the ever increasing use of cross-sectional imaging modalities the incidence of detection of ALL has also increased.
Accessory hepatic tissue can be easily identified and characterized when computed tomography (CT) or magnetic resonance imaging (MRI) of the abdomen is performed for related or unrelated clinical conditions.
Awareness of existence of this anomaly enables early diagnosis by imaging modalities 10,11 Fig. 7.
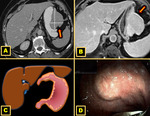
An accessory lobe can simulate a mass in both upper quadrants,
with differential diagnoses including enlarged kidney,
gallbladder,
liver tumor or other abdominal tumors (such as right colonic tumor or gastric neoplasm) 11,12 Fig. 8.
An ALL connected to normal liver tissue can be readily diagnosed based on CT/MRI characteristics,
although diagnosis of a completely separate ALL is less straightforward.
In order to make an accurate diagnosis,
factors such as size,
shape,
position,
presence or absence of related complications (as well as the type of complication) should be considered 11.
CT may aid in establishing the diagnosis of an accessory lobe of the liver by showing the lesion as a soft-tissue density mass attached to the liver and isodense to the organ.
Nowadays it is not common to mistake ALL with lesions of adjacent organs (such as tumors of kidneys,
gallbladder,
pancreas,
spleen,
or adrenal glands,
lymphadenomegaly,
etc.); however,
in cases in which the diagnosis remains doubtful,
correlation with radionuclide scanning may help to reach a definitive diagnosis on the hepatic origin of the mass.
MRI with hepatobiliary contrast media can be performed in an analogous way 6,10,12.
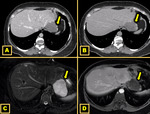
The opposite can also occur: morphological alterations of the liver (such as parenchymal compression by invagination of peritoneum,
or retraction of diaphragmatic muscle bundles and ribs) induce the formation of accessory fissures and lobulations in the contours of the liver (as well as some hepatic exophytic lesions can do),
mimicking ALL 6,10,12 Fig. 9.
Elongated left lobe of the liver
An elongated left lobe (ELL) of the liver is defined when this lobe extends beyond the stomach to the left and / or reaches the superior pole of the spleen on imaging studies 13 Fig. 10.
ELL may be misdiagnosed as distension of the splenic flexure of the colon,
gastroptosis,
hydatid cyst or liver sarcoma.
These elongated lobes may reach up to spleen and may be mistaken for splenomegaly.
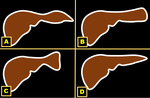
The left lobe of the liver may exhibit various forms: leaf like; spatular; truncated pyramid/ wedge shaped; linguiform; and a bifid appearance 13 Fig. 11.
In opposition,
there is also the absence of the left anatomical lobe of the liver,
an infrequent condition,
which can occur owing to several events,
such as neoplasia,
chronic damage,
trauma,
prior surgical resection,
and agenesis 13 Fig. 12.
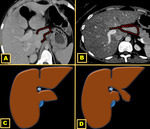
Papillary process versus ALL
The hypertrophic papillary process (PP) is among the main mimickers of ALL.
It may represent only a normal variation of anatomy or occur in the context of cirrhosis owing to enlargement of the caudate lobe 7,14,15.
The caudate lobe is subdivided into Spiegel’s lobe (the caudate lobe proper and the papillary process),
caudate process and paracaval portion,
which is anterior and lateral to the inferior vena cava.
The caudate lobe is connected to the right lobe of the liver by the caudate process,
which passes laterally between the portal vein and the inferior vena cava at the porta hepatis 14,15.
Although it was described in the early 1980s by Couinaud,
the concept of segment IX of the liver should be abandoned because it has no drainage or independent irrigation and the term of paracaval aspect of the caudate lobe has been used more properly 16 Fig. 13 Fig. 14.
The caudate process is sometimes elevated.
The medial inferior part of the caudate lobe may form a papillary process,
which passes left (and also sometimes anteriorly) to the region of the superior recess of the omental bursa.
The caudate and papillary processes are sometimes separated from the remainder of the liver by grooves or fissures 14,15.
For anatomical reasons it is fundamental that radiologists do not mistake a prominent papillary process as being an ALL or even a nodular lesion Fig. 15 Fig. 16.
Complications
Patients with ALL may have overt symptoms or their lives may be in danger if they have complications.
Reported complications include reversion,
infarction,
hemorrhage,
fracture,
compression of neighboring organs,
hemangioma,
gallbladder torsion,
hepatic dysfunction,
diaphragm defects,
and acromphalus Fig. 17.
ALLs may be also associated with congenital biliary atresia,
congenital diaphragmatic defects,
and hepatic cavernous hemangioma 4,5.
A pedunculated ALL carries a higher incidence of reversion in comparison to other types of ALLs.
Severe congestion and blood stasis resulting from an insufficient blood supply vastly increases the incidence of vascular ruptures.
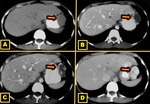
In cases of ALL,
it is not uncommon one complication being joined by others,
such as reversion of an ALL manifesting concurrently with infarction and rupture 17,18 Fig. 18 Fig. 19.
It is easy to foresee the relationship between accessory liver lobes and certain pedunculated hepatocellular tumors.
Effectively,
primary hepatocellular or metastatic tumors have been described in accessory or ectopic lobes.
Pedunculated hepatocellular tumors are rare,
the incidence being estimated to range between 0.2% and 4.2%,
but the incidence is probably under-estimated since the literature reports are constituted of small surgical series 6,18,19.
The association between ALLs and pedunculated tumors has not been clearly shown.
However,
some authors believe that ectopic liver could be more prone to malignant transformation because of metabolic dysfunction.
Although this is a possibility,
one must remember that hepatocellular carcinomas developing on a so-called normal liver (without cirrhosis,
chronic active hepatitis,
or fibrosis) and in the absence of known risk factors is not a rare event 6,18,19 Fig. 20.